To support timely, accurate reimbursement for orthodontic services, use the guidelines below when submitting orthodontic claims to Cigna. Following these steps helps reduce rework and prevent avoidable delays in processing.
Filing Orthodontia Claims
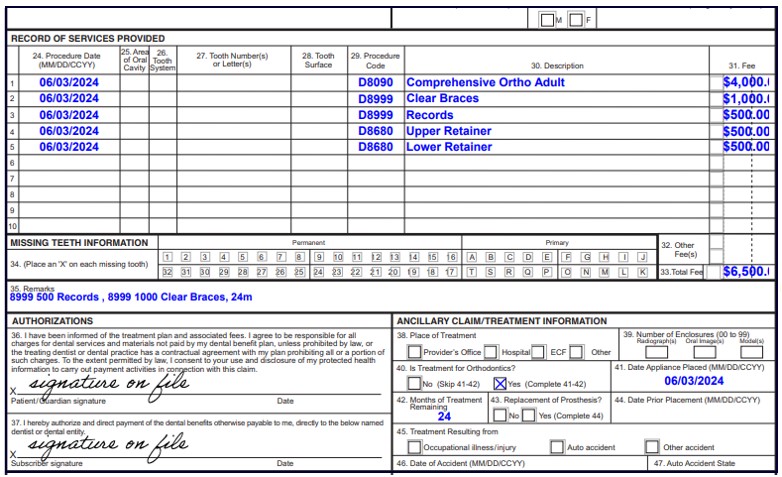
Submit orthodontia claims using your usual and customary orthodontic fees. Cigna calculates orthodontic benefits using the methodology below:
- Records, non-traditional appliances (e.g., Invisalign®, cosmetic or ceramic brackets), and retainer fees are deducted from the total case fee.
- Benefits are paid up to Cigna’s liability for the approved treatment plan or the lifetime maximum—whichever occurs first.
- The remaining amount is used to calculate the initial banding/activation payment, paid at 25%.
- The remaining 75% is issued automatically over the course of treatment on a monthly or quarterly basis.
To ensure benefits are calculated accurately, claims should reflect your full, usual orthodontic fees (not discounted or contracted amounts).
Required Information for Orthodontia Claims
Include the information below with each orthodontic claim to support efficient review and processing:
- A complete treatment description, including the applicable CDT codes
- Dates of service for each line item (unless the submission is a pre-determination)
Please itemize usual and customary orthodontic fees as follows:
- Non-traditional appliance fee (e.g., Invisalign®, cosmetic or ceramic brackets), if applicable
- Total case fee, including:
- Initial banding (or appliance placement) fee
- Active treatment duration (number of months) and associated fee
- Retainer fee (including arches involved)
Providing complete itemization supports accurate benefit calculation and helps prevent processing delays or underpayment.
Ongoing Payments
- Monthly orthodontic claim forms, verification cards, and receipts are not required.
- After the initial claim is processed, Cigna automatically generates future monthly or quarterly payments for covered expenses, based on the approved orthodontic treatment plan.
- If a patient discontinues active orthodontic treatment, notify Cigna promptly to help ensure payment accuracy.
- When Cigna is the secondary payer, include an explanation of payment for every service—including each monthly installment—to support accurate coordination of benefits.
- After treatment is complete, submit a separate dated claim for retainers. Retainer payment is not issued automatically.
Need to update your information—or changing the rendering dentist on an orthodontic case? Please contact your Provider Relations Manager to help ensure active orthodontic treatments are managed correctly.
